Eye pressure is as important an indicator of healthy eye function as visual acuity, color vision, and refraction (refraction) capacity.
What is intraocular pressure
Intraocular pressure (IOP) is the pressure that intraocular fluid (moisture) exerts on the internal structures of the eyeball.
Human eyes constantly produce intraocular fluid. It provides nutrition to the lens and cornea, which lack blood vessels. The fluid circulates between the front and back chambers of the eye and creates pressure inside the eye. When new fluid enters the eye, an equal amount of it must drain out through the drainage system, thin channels in the cornea. If the moisture is produced in optimal quantities and its excess is withdrawn in a timely manner, the pressure remains stable.
The normal ocular pressure is 10-21 mm Hg. Deviations from these values occur with eye disease and can lead to a decrease in visual acuity.
What causes the eye pressure to rise
Ocular hypertension (ophthalmotonus) is an increase in intraocular pressure. It may be temporary or permanent and is directly connected with age: it occurs in 10% of people older than 40.
Ophthalmotonus results from excessive intraocular fluid production or disturbance of its outflow through the drainage canals. Causes of ocular hypertension:
- Glaucoma;
- Eye infections and inflammatory diseases (e.g. uveitis – inflammation of the vasculature of the eye);
- traumas and neoplasms of the eyes and eye orbits;
- long-term use of certain medications (for example, steroid hormones);
- Congenital peculiarities of the structure of the eyes.
High blood pressure, chronic vascular disease, and diabetes mellitus can also contribute to ocular hypertension. Predisposition to high IOP is hereditary.
What are the symptoms of elevated intraocular pressure
Moderate intraocular hypertension is usually imperceptible. The first indicator of increased IOP may be mild discomfort and increased eye fatigue. Symptoms of increased intraocular pressure:
- Pain in the area of the eyeballs;
- Increased sensitivity and redness of the eyes;
- Headache, nausea.
With prolonged persistent increase in IOP, visual acuity decreases. In severe cases, ocular hypertension is manifested by narrowing and loss of fields of vision (blurred areas appear in the field of vision).
What diseases high eye pressure leads to
Increased eye pressure can lead to glaucoma, a disease in which the eye nerve is damaged due to ophthalmotonus. More than 2 million people worldwide develop it each year, and another 6,000 develop permanent blindness. Types of glaucoma:
- Closed-angle – associated with blockage of the drainage system of the eye;
- Open-angle glaucoma – related to disrupted outflow of intraocular fluid through open drainage channels.
Glaucoma is treated with conservative and surgical methods. An ophthalmologist determines the appropriate type of therapy depending on the type and severity of the disease.

Detection of asymptomatic ophthalmotonus and its elimination contributes to the prevention of glaucoma development and preservation of vision. A complete check of the child’s vision also includes measuring IOP. Elevated intraocular pressure in a child may be associated with the development of juvenile (child and adolescent) glaucoma.
How the eye pressure is measured
A distinction is made between true and tonometric intraocular pressure. True pressure is the actual fluid pressure inside the eye. The tonometric pressure is the value obtained by measuring IOP using classical methods (e.g. weights).
The measurement of intraocular pressure is called tonometry. Intraocular pressure is determined during a consultation with an ophthalmologist. Methods of ocular tonometry:
- Contact (the apparatus for measuring IOP touches the cornea);
- Non-contact (a jet of air is used to measure IOP).
The contact IOP measurement with the classical methods begins with anesthetic eye drops put into the eye. With the Maklakov method, weights are placed on the cornea. In Goldman’s method, they drop a staining solution and then a special apparatus presses thin plates to the cornea and determines the pressure level.

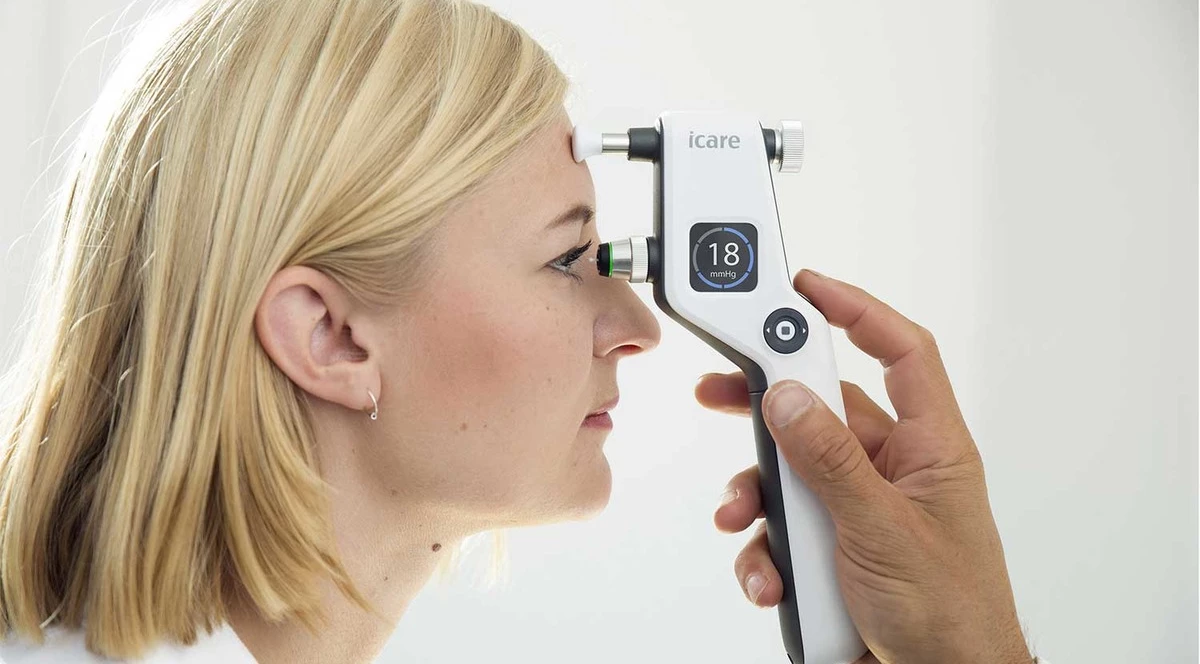
Measuring IOP with modern portable units takes a few minutes and allows you to determine the true intraocular pressure. A device is attached to the person’s eye, which is “shot” with a disposable sterile tip. It touches the cornea for 0.1 second and bounces back into the machine. The measurement is so fast that there is no time for a pain reflex, so there is no need for anesthesia. This is especially important for ophthalmologic examinations of newborns and small children – with other methods of measuring IOP they need sedation.
How to decrease intraocular pressure
Only a doctor can correctly prescribe treatment for elevated intraocular pressure, so if you find symptoms of ocular hypertension, you should make an appointment with an ophthalmologist. With moderate hypertension, an ophthalmologist may recommend observation for several months or lowering IOP with eye drops. Manual or machine eyeball massage may be prescribed by an ophthalmologist as an adjunctive method to normalize IOP.